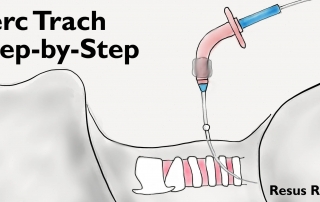
Perc Trach Step-by-Step Tutorial
For patients that require prolonged mechanical ventilation, a tracheostomy can be placed either in the operating room as an open surgery, or more preferably at the bedside with a minimally invasive procedure in the intensive care unit by a percutaneous dilational technique under bronchoscopic guidance. This is a step-by-step tutorial for patient selection and procedure techniques.
Perc Trach Procedure Documentation
Part of performing a bedside percutaneous tracheostomy is the procedural documentation. Given that this is a surgical procedure, the documentation should be more thorough than you may be accustomed to doing for an arterial line or central line. Here is a sample procedure note that can be adapted to your local practice.
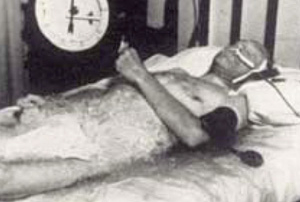
Therapeutic Hypothermia: The History of General Refrigeration (Podcast 02)
The Targeted temperature management Trial compared outcomes for therapeutic hypothermia at 33°C versus 36°C for cardiac arrest patients with persistent coma. It may very well be practice changing. Or maybe not. Before we can figure out what “truth” this research study may have uncovered, we will look at the development of therapeutic hypothermia and what the literature has already told us.
How to Make an Elbow Pad for Olecranon Bursitis
The pain of pressure or bumping an swollen inflamed olecranon bursitis is often quite severe. A foam elbow pad can prevent direct impact and avoid causing additional pain. This how-to tutorial will show you how to make one from materials around your department.
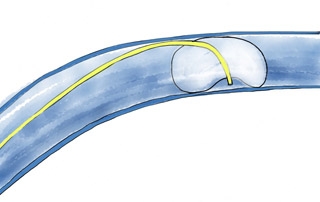
Eccentric Overwedging of a Pulmonary Artery Catheter
Over-wedging of a pulmonary artery catheter can lead to pulmonary artery rupture. This can be caused by an eccentric wedge, which traps the catheter tip against the vessel wall causing fluid to build up increasing the pressure in the trapped cavity.
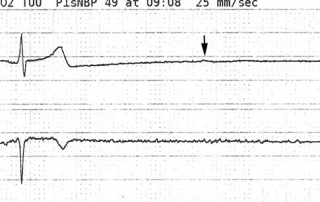
Asystole While Removing a Central Venous Catheter
Transient vagal stimulation from the removal of the CVC and carotid massage from holding pressure to achieve hemostasis can lead to excessive vagal tone which caused blockage of the AV node leading to transient asystole cardiac arrest.

Contribute your thoughts.