A paper by Niklas Nielsen et al titled “Targeted temperature management at 33°C versus 36°C after cardiac arrest”. Published online by The New England Journal of Medicine on November 17, 2013 has brought a lot of attention to the use of therapeutic hypothermia for post-cardiac arrest cares. It stormed through the social media channels. Within days, EMRAP, Emcrit, Life in the Fast Lane, St. Emlyn’s, Intensive Care Network and most other ED/critical care websites and podcasts had devoted time to covering it. It may very well be practice changing in emergency departments and ICUs through throughout the world. Or maybe not. Before we can figure out what “truth” this research study may have uncovered, we will look at the development of therapeutic hypothermia and what the literature has already told us.
Download Episode: ResusReview-Podcast-02-Therapeutic-Hypothermia-History-and-TTM-Trial.mp3
Chapter 1 The Beginning
Ancient societies had long figured out that hypothermia was useful for acute hemorrhage control. But Hippocrates had figured out a way to use the body’s heat production as a diagnosis tool. He would take his patients, and cake them in mud. The areas that dried first were warmer. “In whatever part of the body excess of heat or cold is felt, the disease is there to be discovered.” And once they figured out the diseased are, the proceeded to inflict their “cures” on the patient.
Typhoid fever which had been the plague of Athens in 400 BC and caused the die out of the Jamestown Colony in the early 1600s, led Robert Boyle around 1650 to attempt to cure Typoid by dunking patients in ice-cold brine. While this is likely the first true application of therapeutic hypothermia, it was unfortunately unsuccessful and failed to alter the 30-40% mortality rate of Typhoid. 100 years later James Currie expanded on Boyle’s work to look at the effects of hot, cold, and warm to treat fevers…both by applying it to the surface and having the patients drink it. These innovations did not seem to bring any more success than the ice-cold brine did however. He did find some usefulness from his other work with opium and alcohol for inanition though.
In the early 1800s, hydropaths had become popular though separate from medicine. Osler referred to them as “hermaphrodite practitioners who look upon water as a cure-all”. BUt he realized the hygienic and therapeutic effects of their use of compresses, douches, and baths. Brand, a hydropath from Settin, ended up teach Osler that systematic rigid protocol of cold baths for Typhoid fever did save lives, and Osler implemented this at John Hopkins with success. He published this protocol in an article “The Cold-Bath Treatment of Typhoid Fever” in 1892, and a drop in mortality was seen throughout by physicians everywhere.
During this time, Russian physicians had independently begun using cold for resuscitation. People who suddenly became unresponsive, were covered with snow hoping for return of spontaneous circulation.
Chapter 2 The 1930s and breaking the thermal barrier
This “thermal barrier” was so deeply ingrained into medical techniques at the time that subnormal temperature were to be combated at all cost. All of the clinical thermometers of the time were calibrated down to only 94 F, as the lowest temperature compatible with survival in human being. Below this level, they were confident that human life could not be sustained. Shock cabinets with electrical heating devices or hot water bottles and warm blankets were considered as necessary emergency equipment in every hospital. But this was about to change.
Therapeutic Hypothermia’s father is Dr. Temple Fay. A Neurosurgeon at Temple University. As a medical student one day he was quizzed by his mentor on why tumors were less common in the extremities. He was unable to come up with a reasoned response. This ultimately led him down the path of experimental cancer work. In 1937, he published work on suspending the growth of cancer cells when they were made hypothermic, but their growth would resume normally when normal temperatures were restored.
In a remarkable bench to bedside transition, the next year in 1938, he treated is first cancer patient with hypothermia in an attempt to prevent cancer cells from further multiplying. Chloral hydrate, sodium bromide (both sedatives) were given by rectum the night before. Paraldehyde, another sedative, was given immediately before hypothermia induction. The patient was cooled to 32 deg C for 24 hours, and he was a meticulous record keeper continuously monitoring pulse pressure, Hgb, pH, CO2, urine, blood analysis.
He described it like this.
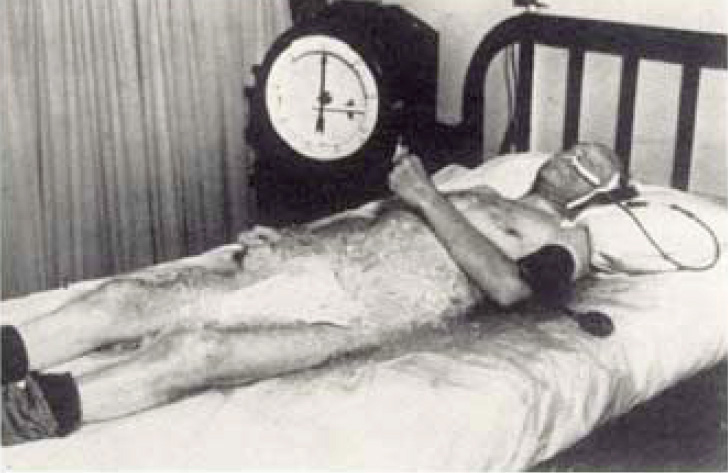
The First attempt at general refrigeration was made on November 28, 1938, which was welcomed as a cool crisp day in Philadelphia. Cool enough so that when I move other patients out of a small four-bed ward, shut off the heat, closed the door to the hall, and opened the winders, Nature herself supplied the cold air that aided the cracked ice, 150 pounds of which was begged from the hospital kitchen. For many reasons, chiefly because of the prejudice on the part of the nurses, we had not dared submerge the entire patient in a bed of cracked ice. As it was, the Superintendent of the hospital was more concerned about the wet mattresses from the melting ice than the scientific principle. The nurses’ home, interns quarters and many members of the staff of other services, were alive with dubious comment and conjecture regarding the idea of human refrigeration.
A series of patients were treated, but the nurses detested working on the “refrigeration service” as they called it.
“Frankly, the nurses were scared: they could not get the patient’s temperature with the clinical thermometers. the long-stem laboratory thermometers might break in getting a rectal reading. The ice and ice water were always in the way, even when the patient was turned. The pulse was weak. The breathing was shallow. I can’t get the patient’s blood pressure. Were all reports that kept the staff in a constant state of alarm. The entire project of general refrigeration had snowballed into a vast issue of distortions of truth, and even my friendly colleagues began to look askance and asked how long was this absurd experiment going to be permitted”.
The program was almost shut down, but Fay and the hospital engineering staff developed blankets made from rubber tubes devised to carry a cold solution from a special “beer cooler” machine pumps were commercially available and were found to be useful in this technique. Also developed electric thermocouples for 24-hour charting of rectal temperatures were also designed. This lead to the disappearance of dedicated cold rooms.
“What we learned after breaking the human thermal barrier on the hypothermic side, was that human survival was possible under proper supervision. When total body refrigeration was established above 24 C and that a hypothermic state could be maintained for 10 days (probably longer if required) when temperature levels of 29.4-32.3 C were maintained.
In addition to his work on cancer treatment, he developed local refrigeration techniques to reduce pain, and In 1945, Dr. Fay was the first to publish a case series on using hypothermia for cerebral trauma.
During WWII, Germans captured one of Fay’s manuscripts “Observations on Prolonged Human Refrigeration” that had been sent to Belgium for publication. German pilots who were downed in frigid waters, would succumb to the freezing temperatures, even if they were rescued quickly. This lead to a series of hypothermia recovery experiments conducted on concentration camp victims, in one of the most grotesque and unethical distortions of medicine. When the German atrocities were discovered, it set back the field by 10 years.
The 1950s saw the expansion of of general refrigeration. A period when great strides were made in therapeutic hypothermia. Bigelow, in 1950, developed and quickly perfected the use of general hypothermia for intracardiac surgery, benefiting both the brain and the heart. In 1954 and 1955, Rosomoff lead a group of bench researchers who worked out much of the physiology figuring out that therapeutic hypothermia reduced cerebral oxygen consumption, blood flow, and metabolic rate. Demonstrated a direct effect between body temperature, and intracranial pressure and brain volume.
Suad Niazi and John Lewis, at the University of Minnesota and Ancker Hospital (Now Regions Hospital) in St Paul Minnesota, worked out first an animals and then in a case report that even profound hypothermia of 9 deg C, was achievable and then was able to be rewarmed with complete recovery. This would impact the treatment for for patients with accidental hypothermia.
The first landmark paper from this period however, is by G Raney Williams and frank Spencer, both from Johns Hopkins, published 4 cases of hypothermia, published in 1959 in the Annals of Surgery. “Clinical Use of hypothermia following cardiac arrest”. This is an absolutely fascinating series of 4 case reports of patients who suffered cardiac arrest, received open chest cardiac massage to achieve ROSC, and then were treated with hypothermia.
38 yo male was admitted to the ED during the evening of September 28, 1957 after sustaining a knife wound of the left chest. On admission he was unconscious and pulseless but was breathing. Neck veins were distended. About two minutes after admission that shallow respirations ceased entirely. Endotracheal intubation and left thoracotomy was performed. The pericardium was distended with blood; the heart was in complete arrest. When the pericardium was opened, bleeding from a laceration of the right ventricle was controlled by pressure while cardiac massage was begun. Good contractions began quickly, and the wound in the ventricle was closed with catgut sutures. The patient was deeply unconscious and unresponsive, with dilated pupils slightly responding to light. There was an increase in extensor tone with hyperactive deep tendon reflexes. Cooling was begun immediately, temperature was maintained at 32-33 deg C. A tracheotomy was performed. Twenty four hours after the injury, the patient would respond to spoken voice and motor power was present in all extremities. At 48 hours there was no neurologic deficit.
This is a resuscitation note that could be written in any emergency department today, 56 years later.
Later that same year, Williams and Spencer, now joined by Donald Benson as the lead author published a larger case series of 27 patients. The paper titled “Use of Hypothermia after Cardiac Arrest.”. Of the 27 pts in this case report,2 failed to get ROSC, 6 had no coma and were excluded from the analysis. Of the 19 remaining, 12 received hypothermia and 7 did not. 1/7 survived in not treated group, 6/12 in hypothermia group (14 vs 50%). They treated at 30-32 deg C from 34-84 hours, and was stopped based on the patient’s response.
By 1959, induced hypothermia was also widely used by neurosurgeons for head and spinal cord injuries as well as during cardiac surgery.
Chapter 3 Lost decades
Despite the apparent success of therapeutic hypothermia, as it moved into more widespread practice the severe complications difficulties with the treatment became apparent, overwhelming its benefits. Cardiac irritability and ventricular fibrillation when patient’s temperatures were below 30°C, which was a problem because the accuracy and precision meeting a target temperature with the available equipment was nearly impossible. There was a much higher rate of infections, most significantly a decreased clearance rate of staphylococcal bacteremia. There were additional problems with vasospasm, increased plasma viscosity, hyperglycemia, cardiac dysfunction, and coagulopathies.
So, even though there were clear protective effects of therapeutic hypothermia during brain ischemia and head injury, it became apparent that the complications of this therapy made its use risky, and very difficult to manage without intensive care. The technique was essentially abandoned.
Chapter 4 Resurgence
So hypothermia was put on a shelf. Not forgotten, labelled a once promising therapy that failed to be benficial. There were periodic papers published after 1960, but much of it focused on techniques in cardiac surgery, or basic animal model work.
The few human papers on therapeutic hypothermia published during this time, only reinforced the downsides of hypothermia. In 1986, Bohn published a case series of 24 children resuscitated after drowning who remained in persistent coma. They were treated with therapeutic hypothermia to treat elevated intracranial pressures. Those treated with hypothermia had a much higher rate of neutropenia and septicemia, than the control group.
Cardiac arrest care, however, advanced during this period. Zoll published his work on externally applied counter shocks for ventricular fibrillation. 1960 and 61 saw Kouwenhoven and Safar introduce closed chest massage. The 70s and 80s saw the development of the cardiac arrest care systems. Mobile defibrillator units were developed in 1979. “The White Paper” in 1966 by the National Academy of Sciences spurred the development of EMS systems across the country. Cummins, Ornato, Thies, and Pepe published their “Chain of survival” concept in 1991, along with the american heart association. With CPR and defibrillators now available out of the hospital and in the field, and trained personnel there to tend to the patients, the possibility of widespread early resuscitation from cardiac arrest became a reality.
Disappointment set in again though. Despite the improvements in cardiac arrest care, patients continued to do poorly. Only a tiny fracture were surviving, and of those that did, they were suffering profound neurologic recovery. Becker in Annals of Emergency Medicine, summed up frustration with their paper titled “Outcome of CPR in a large metropolitan area-where are the survivors?”
The same year 1991, Frtiz Sterz published a large animal study in dogs that showed that mild hypothermia initiated immediately after return of spontaneous circulation, improved neurologic outcomes. The target of 34-36 deg C was unique in its temperature target, and several degrees warmer than the 32-33 deg C of much of the earlier literature. more than that, the maintained the target temperature only for 1 hour post-resuscitation, and then let the temperature climb passively.
With abilities to resuscitate cardiac arrest patients, it was felt better post-arrest cares would improve outcomes. So researchers turned to therapeutic hypothermia. In 1996 alone, Sterz published a major review article, Peter Safer, who had developed closed cardiac massage published a major animal study using hypothermia, Stephen Bernard published a major review in the Anesthesia critical care literature, and a Symposium was held at the Society of Critical Care Medicine conference on hypothermia.
Chapter 5 Hypothermia becomes the Golden Child
The next year, 1997, was the first of two landmark papers by Stephan Bernard and colleagues from Monash Medical Center in Australia. Published in Annals of Emergency Medicine, “Clinical trial of Induced Hypothermia in Comatose Survivors of Out-of-Hospital Cardiac Arrest”. This was a pilot study and the followed 22 patients prospectively with 22 retrospective matched controls. They treated the comatose resuscitated patients at 33 deg C for 12 hours. Mortality was 10 vs 17, and CPC 1 or 2, was 11 vs 3. In 1998, Yanagawa and Zeiner in 2000, published similar small pilot studies which also showed the promise of improved outcomes.
Peter Safar summarized the history and state of therapeutic hypothermia in 2000 commentary in Academic Emergency Medicine. Brilliantly title “On the future of reanimatology”, it ended by calling for a randomized control trial.
Two groups working independently answered this call. In 2002, their results of their work were published in the same issue the New England Journal of Medicine.
Stephen Bernard and his colleagues, had expanded on their earlier paper. Titled “Treatment of Comatose Survivors of Out-of-Hospital Cardiac Arrest with Induced Hypothermia”, they prospectively randomized 77 patients with resuscitated VF with persistent coma. They excluded pregnancy and persistent cardiogenic shock despite epinephrine. All received lidocaine. The MAPs were maintained between 90-100 mmHg, pO2 > 100, pCO2 of 40. Patients were cooled to 33 deg C for 12 hours before being allowed to passively rewarm. Mortality was similar in both groups, but patients with CPC 1 or 2 was 21 vs 9 if they had been treated with hypothermia.
The second study was conducted in Austria. “Mild Therapeutic Hypothermia to Improve the Neurologic Outcome after Cardiac Arrest”. Enrolled 237 patients with resuscitated ventricular fibrillation arrest who were treated with therapeutic hypothermia to 32-34 deg C fr 24 hours compared to patients with normothermia. Median time to starting cooling was 105 minutes post-arrest, but the patients did not reach target temperature until nearly 8 hr after arrest. the was a 14% absolute risk reduction in mortality and 16% improvement in CPC 1 and 2 scores for patients treated with hypothermia. Overall a remarkable benefit.
Based on the strength of the previous smaller studies by Bernard, Yanagawam and Nagaeo, and these two larger papers, hypothermia was endorsed as a recommended treatment first by the American Heart Association in 2002, and then in 2003 by Advance Life Support Task Force of the International Liaison Committee on Resuscitation.
Therapeutic hypothermia was considered a settled question, and its use in post-resuscitation cares spread widely and quickly as a standard of care. It was incorporated into all manner of guidelines. But settled questions in medicine are rarely so.
As the practice became more widespread, areas of controversy developed. Treatment was expanded to resuscitated rhythms other the ventricular fibrillation and ventricular tachycardia, under the assumption that brain ischemia from any source would benefit from hypothermia. The optimal temperature target was also uncertain. Guidelines had adopted 32-24 deg C, which had been the traditional target as we have talked about.
Work at the Peter Safar Center for Resuscitation in Pittsburgh lead to a paper published by Eric Louge and Clifton Callaway in 2007 in Academic Emergency Medicine. “Comparison of the Effects of Hypothermia at 33 or 35 after Cardiac Arrest in Rats” They were able to demonstrate the minimal hypothermia at 35 deg C was just as good as cooling to 33 deg C in terms of mortality and neurologic outcomes, and both performed better than normothermia.
Zeiner published data that a fever in the post-cardiac arrest period had adverse neurologic outcomes. So researchers postulated that the neurologic benefit has little to do with hypothermia, and is the result of prevention of hyperthermia. We are back to improving the mortality of Typhoid patients by preventing their fever by making them cold.
This was the setting in which the Targeted Temperature Management paper by Nielsen et al paper was introduced. They enrolled 950 pts in 36 centers in Europe and australia, who suffered a resuscitated out-of-hospital cardiac arrest who remained unconscious. Any initial rhythm was allowed which is in-line with current practice. They were randomized to temperatures of 33 or 36 deg C for 28 hours, and the rewarmed. Normothermia was then maintained until 72-hours post-arrest. There was a non-significant 2% mortality difference at the end of the treatment protocol and 180 days later. Patients with CPC score 3-5, was 54 vs 52% and also was not statistically significant.
But was this a definitive non-inferiority study on the temperature target question. That was the resounding initial comments from many, though a strong cautionary post by Dr. Simon Carley at St Emlyn’s blog keeps the study results in perspective. I really encourage you to read it. He points out that the study is powered to find an 11% absolute risk reduction between 36 and 33 deg C, which would be a NNT of 9. That is asking a lot.
So here we are. What would Osler do? How would Drs Temple Fay or Peter Safar treat there next resuscitated cardiac arrest patient. There is no doubt that the critical care involved in maintaining a patient at 33 as compared to 36 is much larger. The risks and complications are higher. Is there benefit. Do more patients benefit? Are more better off neurologically? Hypothermia does seem to convey benefit as compared to normothermia, and certainly to patients who develop a fever. Actively maintaining the temperature at goal for the duration of the treatment seems reasonable. As for the temperature. 36 degrees C has support for the new standard. With increasing NNT, there may be benefit to going lower but with diminishing returns in return for more adverse events. Duration of treatment remains murky in my mind, but 24 hours is my current practice.
As every paper states in their conclusion…more research is needed. I think I got the new issue of Resuscitation in the mail today. I wonder what we will find.
Until next time, stay cold…or cool. This is Charles Bruen, with Resus Review.
[…] came with his fascinating blogpost/podcast putting the latest studies in historical perspective: Therapeutic hypothermia: The history of general refrigeration. Meanwhile I’ve been involved in discussions via Google Hangouts, reading what the big […]
[…] came with his fascinating blogpost/podcast putting the latest studies in historical perspective: Therapeutic hypothermia: The history of general refrigeration. Meanwhile I’ve been involved in discussions via Google Hangouts, reading what the big […]
[…] Bruen. Charles puts the recent theraeutic hypothermia studies in there historical context in Therapeutic hypothermia: The history of general refrigeration. […]
Charles, this website is AWESOME (and you know I’m way too old to use that word).