Intubations can be difficult for numerous reasons, but in my mind the most frustrating circumstances is when you have the trachea cannulated (either by open tracheostomy or perc trach) and are unable to pass the endotracheal tube. This occurred to me on a recent patient.
Case Description
The patient was a 69-year-old woman nursing home resident who was admitted to the ICU with right lower lobe pneumonia and early sepsis. On admission she had only mildly respiratory. She was treated aggressively with fluids and antiinfectives, and stabilized quickly. However, during the first day of her ICU stay her respiratory status worsened and she ultimately developed hypoxemic respiratory failure requiring orotracheal intubation.
She was preoxygenated with 100% noninvasive bilevel ventilation. Per protocol she was quickly assessed prior to intubation.
- BVM ventilation Risk: Moderate
- good mask seal
- no obstruction
- no tongue edema
- obesity
- advanced age
- many missing teeth
- moderate airway pressures
- Intubation Risk: Moderate
- Gestalt
- 3 finger widths
- Mallampati II
- Previous intubation and tracheostomy
- Latero-rotational torticollis
She was given etomidate 20 mg and succinylcholine 200 mg.
On the first attempt, under direct laryngoscopy a gum elastic bougie was visualized passing through the cords. It passed easily and was able to be advanced to the carina. The 7.5 mm ETT was passed over the bougie and through the vocal cords, but stopped about 1-2 cm below the cords and was unable to be advanced any further. The endotracheal tube was rotated through a 180° turn and was still stuck. The attempt was stopped, and she was able to be BVM ventilated easily. A repeat attempt was made with a video laryngoscope and a 7.0 mm endotracheal tube, with identical results of the endotracheal hanging up below the vocal cords. On the third attempt, a 6.5 mm ETT was passed over a bougie and into the trachea using very firm pressure.
This was a difficult intubation. During the intubation, the patient’s supraglottic space appeared normal and cannulation of the vocal cords was easy, but placing the endotracheal tube proved frustrating. We were unclear of the reason. Her SpO2 nadir during the intubation was 85%, and once the cuff was inflated and placed on mechanical ventilation there was no air leak and the patient was easy to ventilate.. She was treated for her pneumonia and sepsis, and on hospital day 4 she was extubated. During the extubation, microdirect laryngoscopy of the trachea revealed a stenosis in the subglottic space. This can be seen in the figure below, and is the white fibrotic material just past the vocal cords.
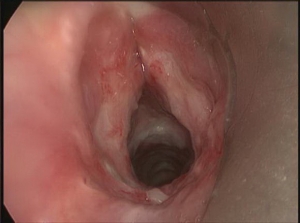
Direct laryngoscopy view of the vocal cords with tracheal stenosis evident in the subglottic trachea.
Causes and Prevention of Tracheal Stenosis
Tracheal stenosis affects 4-13 % of adults after prolonged intubation in United States. The causes of adult tracheal stenosis include trauma, chronic inflammatory diseases, benign neoplasm, malignant neoplasm and collagen vascular diseases. The most common cause of tracheal stenosis continues to be trauma, which can be internal (prolonged endotracheal intubation, tracheostomy, flame burn injury) or external (blunt or penetrating neck trauma). Approximately 90 % of all cases of acquired chronic subglottic stenosis result from endotracheal intubation or tracheostomy.
The cuff-pressure of endotracheal tubes plays an important role on the development of tracheal damage in intubated patients. To minimize this injury, use of high volume and low pressure cuff endotracheal tubes are advocated. When the cuff pressure exceeds the mucosal capillary pressure (30 mm of Hg) of the trachea, the mucosa that lies between the cuff of the balloon and the underlying cartilages develops ischemia. Long standing ischemia can lead to ulceration and chondritis of tracheal cartilages, followed by fibrotic healing leading to progressive tracheal stenosis. Usual factors responsible for stenosis are: cuff pressure, size of the tube relative to tracheal lumen, duration of intubation, cardiovascular status during intubation, movement of tube during the period of intubation, sex and age of the patient, material of the cuff and the possible adverse effects of steroids. However, tracheal stenosis can also develop by intubation lasting as short as 24 hours only.
Our patient had an old tracheostomy which had been decannulated about 5 years prior. She had developed tracheal stenosis at this site. Ultimately, she required permanent tracheostomy.
There are excellent videos on airway management by Dr. John McGill available at hqmeded.com

[…] Bruen on Resus Review discusses an unexpected difficult intubation due to a case of subglottic tracheal stenosis. […]
Thought I would share:
You didn’t mention Idiopathic Tracheal Stenosis (ITS). There is a large population of mainly women that have idiopathic tracheal stenosis. I recently had a tracheal resection and reconstruction, after having 12 dilations for my airway in less than 3 years. Diagnosed in 2009, randomly started having symptoms couple weeks after half marathon. Some speculate acid reflux, maybe hormones, but really no straight forward answers. Just for people to keep in mind that there really is this category of “idiopathic” and not all subglottic stenosis results from the above causes. ;) One ENT I have encountered believes it’s a 100% in women. Who knows, maybe hormone correlation?? I personally have not come across a male that has ITS.
I was 24 yrs of age when I started to have symptoms. From cases I have come across, most people are misdiagnosed with asthma. Treatment for ITS can vary depending on practitioner. For example, lasers (yag/ co2) can be used, balloons, biopsy forceps, stents (not a good option), trachs (really bad situations, especially w/ patient with tracheomalacia), mitomycin ointment, steroid injections, tracheal reconstruction/resection (R&R), rib grafts, tracheal transplant (ex: stem cells). If the scar tissue is too close to the vocal chords or if it integrates into part of the vocal chords, the individual would not be a candidate for a tracheal R&R. If the tracheal segment was long, they too would not be a candidate for tracheal R&R. I had close to 1.25 inch removed. Feeling fortunate.
Just some information that I felt was note worthy of your blog. Love listening to the podcast. Great material;) Thanks
Thanks for the great discussion on idiopathic tracheal stenosis. It is not on my differential much, but it should be.
[…] Difficult intubation caused by subglottic tracheal stenosis – Resus Review — Read on resusreview.com/2013/difficult-intubation-caused-by-subglottic-tracheal-stenosis/ […]