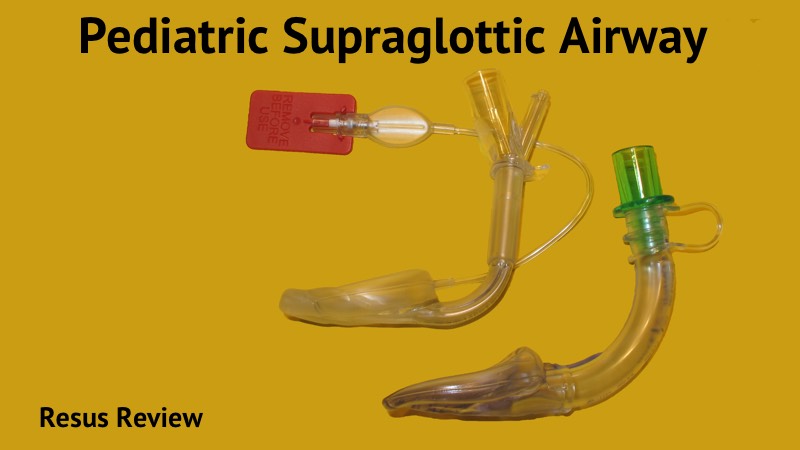
There are numerous critical differences in managing the pediatric airway. There are anatomical differences, especially in children <2-years of age. The child’s head is much larger in proportion to their body than adults, with a large occiput which often requires position of padding behind the shoulders. The airway is also very anterior to what you are used to in adults. Given the small size of the airway, they tend to obstruct much easier, and the stimulation and pain of a resuscitation can lead to dynamic obstruction. There are physiologic differences. Child have a much higher base line oxygen consumption rate than adults and small proportional functional reserve capacity (FRC) which leads to quicker desaturations. Lastly, all medications require weight-based dosing.
While BVM ventilation, direct/video laryngoscopy (including the speciality pediatric blades) are foundation of managing the pediatric airway, the primary backup airway adjunct are the supraglottic devices. In some situations they may be useful for primary BVM ventilation.
Supraglottic airways (ie SGA, Laryngeal Mask Airway, LMA) are available in non-intubating and intubating pediatric sizes. They are sized by patient weight (which is on the device packaging) from newborn to adolescent. The reason for having both intubating and non-intubating SGAs is because both types have unique features that may be critical in a given situation. Below we will discuss which device to choose and why.
Non-intubating LMA Supreme
With infants, we can usually provide adequate Bag-Valve-Mask ventilation with an appropriately sized face mask easily. In a short time however, the stomach becomes insufflated which compresses the lungs and makes it difficult to provide adequate ventilation. This is the main problem we get into with infants.
When you are having trouble with face mask ventilation and/or the patient’s stomach is inflating during face mask ventilation, pick the non-intubating LMA Supreme and use the gastric port to empty the air out of the stomach as ventilation is ongoing. This approach allows us to ventilate through the LMA for a prolonged period without inflating the stomach. Simply remove the LMA when you have provided enough preoxygenation based on the oxygenation saturation level, and attempt your intubation. I think this is the greatest use for peds LMAs, so get used to this device. You can also use this device as the initial first-line ventilation device (instead of BVM ventilation) for newborns and infants, since it usually provides better ventilation than BMV.
They are available in sizes 1, 1½, 2, and 2½.
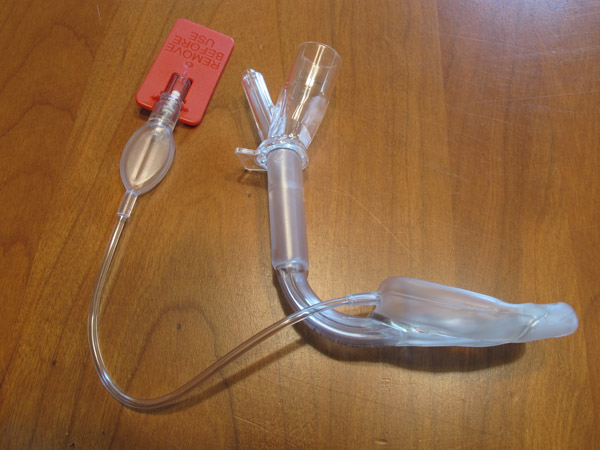

At the top of the LMA Supreme are two ports. There is a standard 15mm ID x 22mm OD adaptor that connects to a BVM or ventilator. There is also a separate channel for a suction catheter that leads to the esophagus.

The figure below shows a detailed view of the mask. At the tip of the mask you can see the exit port for the gastric suction catheter. Notice that the cross-section of the air exit port in post has an upside down U-shape to accommodate the channel for the suction catheter. This makes it difficult to pass a bougie or intubating catheter through.

air-Q Intubating LMA
For a pediatric patient with difficult airway anatomy in which you want to intubate with a bronchoscope, then the preferred approach to use is the intubating air-Q LMA. This device has been tested head-to-head against other pediatric supraglottic airways and is able to accept an appropriately sized endotracheal tube for all patient sizes.

Notice in the photo above, that there is no inflation mechanism (ie syringe adaptor, pilot balloon, and connector tubing). The model shown is self-pressurizing, designated as the “air-Qsp”. The mask is connected to the airway conduit, so it is inflated every time inspiratory pressure is applied either by a BVM or ventilator. It the becomes deflated during exhalation. The theory is that this prevents over-inflation of the mask causing high cuff pressures and subsequence mucosal injury.
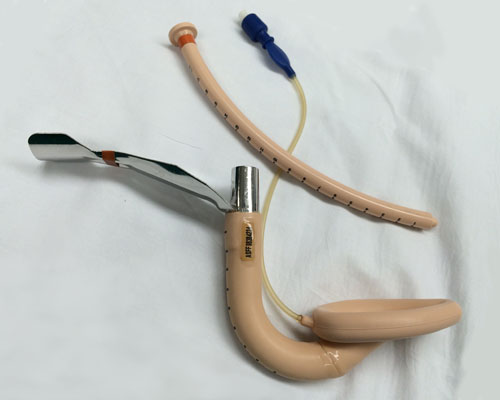
In the oblique view below you can see the large bowel, epiglottis elevator/stabilizer, and central channel that allows for ventilation and passage of an intubating endotracheal tube. Unfortunately, as compared with the LMA supreme there is no suction port.

A unique feature of the air-Q intubating LMA is the removable cap. With cap attached, it is a standard 15mm adaptor. When you disconnect the cap, the central channel is exposed which allows for passage of the endotracheal tube.


Blind intubation through these devices can be difficult, so I would not recommend it especially in an unstable patient. Use a pediatric bronchoscope. They have a diameter of 4 mm and can fit through a 4.5 or larger endotracheal tube. If your patient can handle a 4.5 ET tube (about 12 months of age and above), you now have a way to intubate in a controlled manner using a bronchoscope.
Push rods for removal of the air-Q LMA after intubation are available, but it is generally easier and faster to just use a second ET tube as a push rod.
Fastrach Intubating LMA
The Fastrach Intubating LMA is available in a size 3, which is useful for older children. it is indicated for patients weighing 30-50 kg (approximately age 10-14). The rigid shape works extremely well for seating the mask in the hypopharynx, and is reuseable. It is my preferred intubating LMA for adults and preteens.
Airway Cart
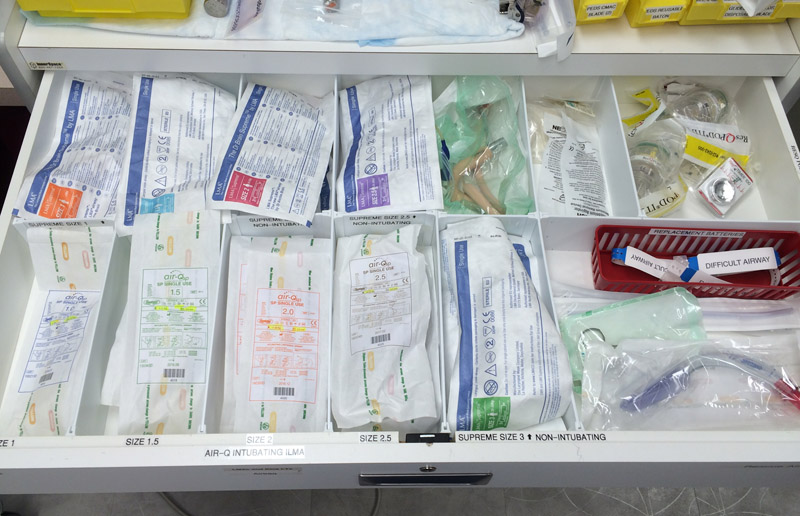
Given the need for various sized tube, a well planned airway cart is a must for fast access and ease of restocking. The figure below is the pediatric airway cart in our pediatric resuscitation bay. It contains all of our equipment, and is labelled so that missing items can be quickly identified and restocked.
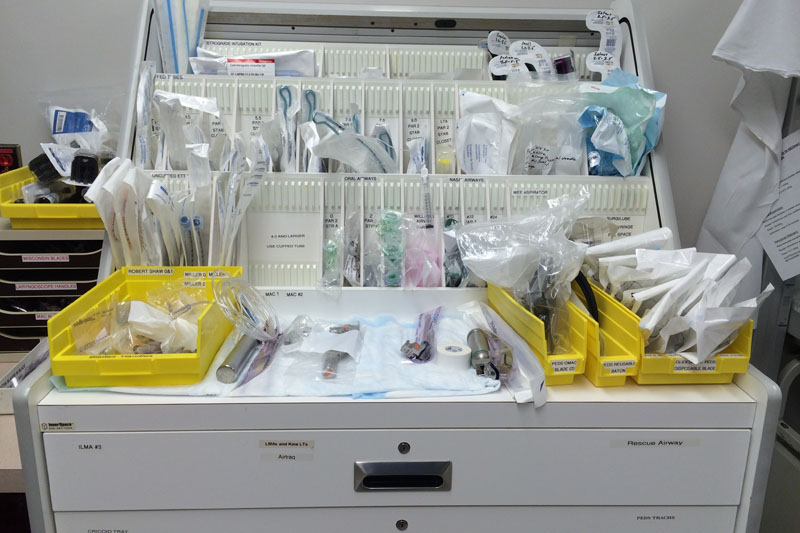
We have arranged the top drawer of the cart to contain the supraglottic airways. It contains the four available sizes of the air-Q LMA, and five sizes of the LMA supreme. It also has a size 3 Intubating Fastrach LMA. As you can see, any misisng devices are easily identifiable.
Conclusion
As we know from our experience with the ILMA in adults, having these devices readily available (and knowing how to use them) is critical to optimizing the safety of pediatric airway management. I highly encourage using these devices on straightforward patients before you are forced to use one in a difficult or failed airway.
For additional airway tips and techniques, please visit HQMedEd.com. Courtesy of Rob Reardon, MD, Hennepin County Medical Center.
Contribute your thoughts.