Preventing sternal wound infections in the post operative cardiac surgery patient is an important aspect of post operative care. Sternal infections can increase length of stay, be a substantial financial impact, and increase mortality’ Occurrence of sternal infections is rare and it has been reported as 0.4–4%.
Managing hyperglycemia post-operatively has been one intervention implemented to make a significant impact on reducing sternal infections. It is for this reason we manage such glucose control for these patient and why glucose control <200 mg/dL by POD 1 and POD2 is part of the Surgical Care Improvement Project. Our most recent data has shown that we have met the 100% mark for maintaining glucose control for this patient population. This is excellent work and is a tribute to the excellent post operative nursing care.
Question have come up with the recent changes to the Epinephrine/Insulin glycemic management. Epinephrine is a natural catecholamine produced in our body by the adrenal glands (endocrine gland on top of the kidney). Production of epinephrine and conservation of glucose is a parasympathetic action to prepare our body for “fight” or “flight” stress situations. Epinephrine stimulates the liver to produce glucose by glycogenolysis and gluconeogenesis. Additionally, Glucagon (hyperglycemic hormone) and Cortisol (steroid hormone) are also contributors to hyperglycemia in stress induced states impacted by epinephrine.
Epinephrine interacts with cellular receptors and sends messages from cell to cell to inhibit insulin, elevate glucagon, and manages glucose utilization or conservation.
For these reasons when Epinephrine is infusing, glucose checks are essential. Most likely if the drip continues an insulin drip will follow. The Epinephrine infusion order in Epic indicates checking glucose every 30 minutes to address Hyperglycemia and Hypoglycemia when titrating epinephrine. This frequency of glucose checks is to help us reach goal of <200mgdL.
However, if a patient is on epinephrine and glucose has stabilized within a normal range for a significant amount of time (i.e. 48 hrs with or without insulin infusing) consider revising the frequency of glucose checks. Start at 2 hours. Be sure to get an order so this change in practice is communicated to everyone. From there on, the glucose checks can be modified further.
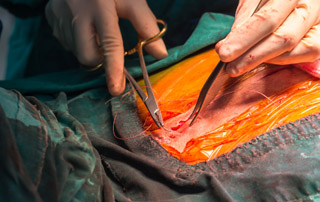
If situations do progress into an infection state there is potential for opening of the sternum to allow for debridement and dressing changes. Often times patients are intubated and brought into the OR for sternotomy and packing. Sometimes patients are paralyzed for prevention of coughing or major movements by the patient. Abrupt movements or major position changes can create a situation where the separated ribs could puncture the ventricles of the heart. Additionally the ribs and the sternum can become malpositioned and may impact closure of the sternum.
The Z-flo pillow is a perfect option for repositioning patients with open sternums and preventing skin break down. Z-flo pillows are great for microturns and off loading pressure in small areas. Additional things to consider for the open chest patient are:
- Log rolling the patient
- Minimize suctioning
- Minimize coughing (these would create pain and opportunity for piercing the heart)
- Promote pain control (PCA)
- Optimal Sedation with paralytics
- Skin assessment
- Low air los mattresses
- Promote perfusion.
References
- Sternal wound care to prevention infection in adult cardiac surgery patients. Critical Care Nurse Quarterly. Jan-Mar;35(1):76-84.
- The effect of tight glycemic control, during and after cardiac surgery, on patient mortality and morbidity: A systematic review and meta analysis. Journal of Cardiothoracic Surgery, 2011;6(3):1-7.
- Effect of epinephrine on glucose metabolism in humans: contribution of the liver. American Journal of Physiology Endocrinology and Metabolism. 1984;24(2):E157 -165.
- Studies on the mechanism of epinephrine-induced hyperglycemia in man: evidence of participation of pancreatic glucagon secretion. Diabetes 1976;25(1):65-71.

Contribute your thoughts.