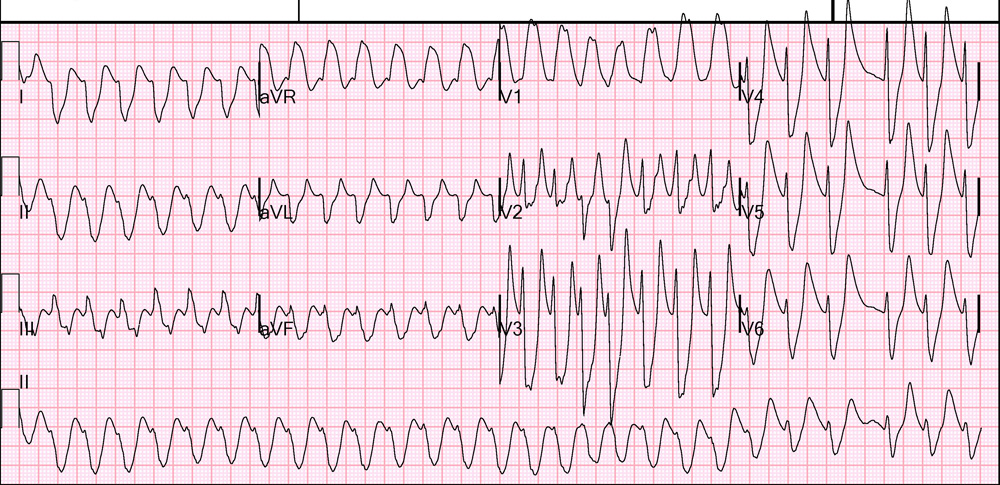
29-year-old man with history of type 1 diabetes mellitus and currently living in a hotel, presented to the emergency department with 2-weeks of feeling ill with had accelerated and was much worse over the last 2 days. This included a productive cough, subject fevers, and frequent vomiting. He was brought in by his brother, and the patient was appeared ill, was somnolent, confused, and only oriented to self. his blood pressure was 78/43 mmHg, pulse 146 bpm, respiratory rate 26, 37.2deg C, SpO2 96%. An finger stick blood glucose measurement read HIGH. A cardiogram was also obtained.
This is a regular wide complex tachycardia. the first question you need to to determine in these cases is if the patient is stable or unstable. In this situation, the patient was hypotensive with altered mental status. He was electrically cardioverted using the synchronized setting and a voltage setting of 150 J. He was then immediately given 3 ampules of calcium gluconate and 3 ampules of sodium bicarbonate.
This is the correct treatment. The physicians inferred from the severe hyperglycemia that the patient may be hyperkalemic, which was the cause of the wide complex tachycardia. given that he was unstable electrical cardioversion was the first step, quickly followed by calcium to help stabilize the myocardium. The bicarbonate is given to facilitate the intracellular shift of potassium. The patient was additionally treatment with 2 L 0.9% saline bolus, 10 units SC insulin aspart were given.
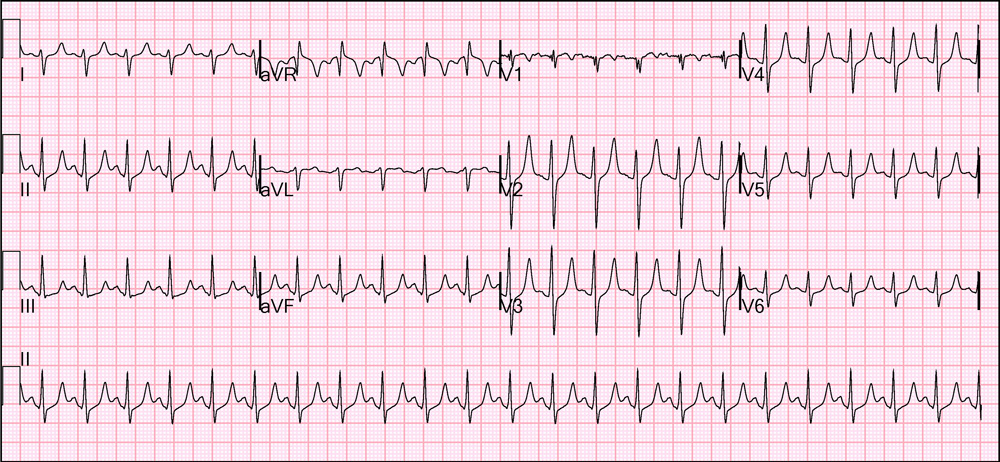
Immediately after cardioversion the following cardiogram was obtained.
What is most impressive is the peaked T-waves consistent with hyperkalemia. His chemistry panel eventually returned which showed at presentation he had a glucose of 1120 mg/dl and a potassium of 6.6 mEq/L.
Androgue (Medicine 1986;65(3):163) created a formula to predict the potassium at admission in DKA.
K+ = 25.4 – (3.02 x pH) + (0.001 x glucose) + (0.028 x Anion Gap)
However in our case it under predicts the potassium, however the paper gives an excellent reviewing he mechanism of hyperkalemia in hyperglycemia.
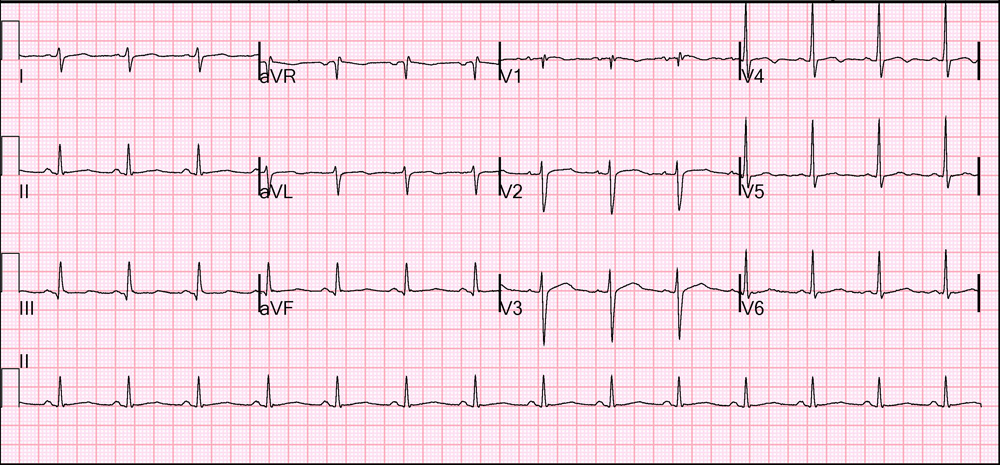
Unfortunately the patient’s mental status did not improve significantly, and ultimately required orotracheal intubation and mechanical ventilation. He was admitted to the MICU where he continued on an insulin protocol overnight. About 10 hours after admission his anion gap had closed, and he was transitioned to long-acting insulin glargine. A repeat ECG at this time showed return of a normal sinus.
The patient ultimately did well and was discharged from the hospital.

whats about DKA management ????
Hi Sir, please forgive my ignorance. If we know clearly from the presenting history and rapid bedside evaluation that the WCT that we are seeing is due to severe life threatening hyperkalemia and not unstable VT, was the synchronized shock indicated in the first place?
Yes, because the patient was hemodynamically unstable.
Hi CYC,
Very good question. If the patient has a WCT rhythm but is stable (good hemodynamics, normal mental status, adequate urine output, no chest pain or shortness of breath), it would be be reasonable to treat the underlying DKA and and keep the parient under close clinical monitoring with telemetry.
On the other hand, most emergeny physcians including myself are uncomfortable with a patient in WCT given the risk of decompensating to an unstable rhythm.
However, this patient was unstable. Hypotension, tachycardia, and altered mental status. This is a clear indication for electrical cardioversion.
Thank you for reading.
Charles Bruen
In answer to above comment: Yes, the patient also had atrial fib with Rapid ventricular response and was in shock. Electrical conversion was perfect, then treat the hyperK.
Teach me: How is that a-fib in the initial ECG? Very regular rhytm, methinks. Cardioversion seems warranted if VT or a-fib but a ST with wide QRS wouldn’t benefit from DC, right? Was it not the calcium and correction of hypovolaemia that did the trick?
On the other hand, if that second ECG was immediately after the shock and without the bicarb and calcium on board I’m obviously mistaken. DC in the unstable patient would be indicated even if unsure of underlying rhythm I suppose. Good job in any case in this sick pt.
[…] DKA presenting as Wide Complex Tachcyardia – Start the insulin and check the K! […]