She had just left the hospital, and had so many scheduled doctor’s appointments over the next several weeks that the last thing she wanted to do was going to the emergency department. There were things to do around the house…shopping, cleaning, mail. Friends were coming over. But the chest pressure that had starting after waking up this morning would just not stop.
This 70-year-old woman had been through a lot recently. She had suffered with aortic stenosis for many years. After long talks with her many physicians and surgeon and a carefully considered pro/con list, she had agreed to undergo surgery. She underwent an surgical aortic valve replacement with a bioprosthetic valve. She had planned her surgery thoroughly. She knew what to expect on getting to the hospital, the day of surgery, and what each day after surgery would involve up to her expected discharge on POD #4. Her planning had comforted her, and gave her control of the situation. At least perceived control.
She had been home from the hospital for 3 days, when the chest pressure had started. Unwilling to call it pain or quantify it beyond “its there”, it was ultimately her daughters (with their own lists of worrisome symptoms from the surgeon), that forced her to the ED. She had also experienced some lightheadedness and nausea.
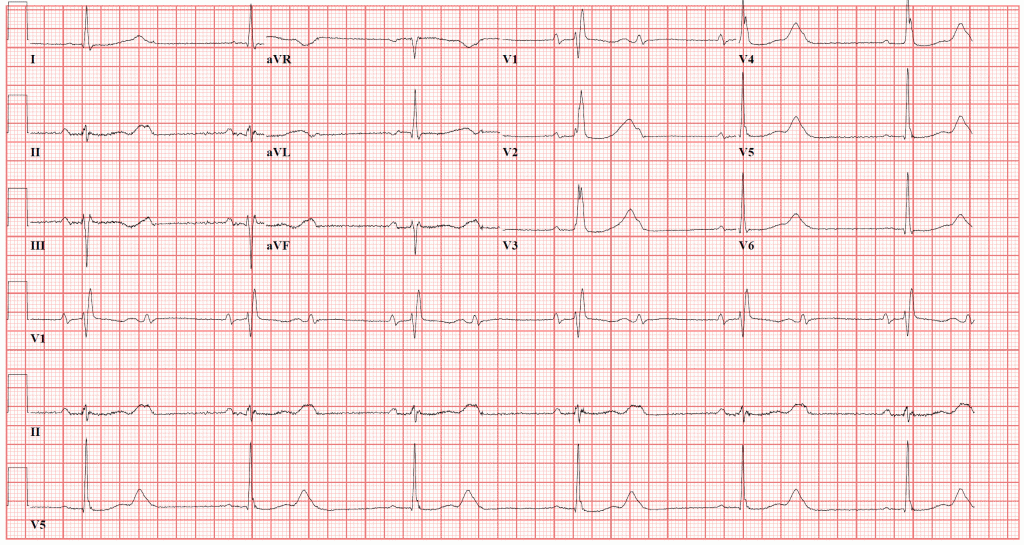
The ECG shows a bradycardia at rate of approximately 36 bpm. There is a right bundle branch block. P-waves are present and occur at regular intervals. There are also non-conducted p waves. The PR interval of the conducted p-waves remains constant and is at the high-end of normal (~200 ms). Most importantly the RR interval of the around the dropped QRS complexes is a multiple of the conducted beats. This is second-degree atrioventricular block, type II (Mobitz). This along with complete heart block (3rd degree), are colloquially called high-degree AV block because of the risk of degenerating.
The ECG does not demonstrate ischemic features (dynamic T waves, T wave inversions, ST segment elevation or depression, QT prolongation). New onset bradycardia and conduction blocks should always prompt you to consider ischemia. In this particular patient acute coronary syndrome would be unlikely. Patients who have planned valvular heart repair, undergo coronary angiography to identify comorbid obstructive atherosclerotic disease. This is so coronary bypass surgery could be done at the same time as the valve surgery. Since she had isolated AVR, we could conclude that her coronary artery disease burden is low significantly reducing, though not eliminating the likelihood of acute plaque rupture.
Unfortunately the development of high-degree AV block after aortic valve surgery is a known significant comorbidity occurring in 4-8% of patients. Chronic aortic valve disease leads to changes in the myocardium and conduction system. Risk factors for developing heart block after isolated aortic valve replacement are:
- Female gender.
- Annular calcification. Increases risk underlying conducting system.
- Presence of pre- or post-operative bundle branch block (RBBB/LBBB). If the conduction system already exhibits bundle branch block, relatively minor operative injuries can precipitate complete block.
- Prolonged cross clamp time which is a marker for myocardial ischemia and injury.
- Preoperative valvular regurgitation. Along with a dilated proximal aortic root is another indicator of cardiac structural abnormalities that can impact the conduction system.
The key decision making in these patients is the timing of implantation of a permanent pacemaker (PPM). We generally delay until at least POD#5, because in the early postoperative period there are many transient conduction abnormalities. Indications that the heart block is irreversible and a PPM is needed are:
- Complete heart block
- Symptomatic bradycardia
- Bradycardia while controlling tachyarrhythmias at day 7
While waiting to at least day 5 is recommended, the mean time to placement 13 days.
It is critical to search for any medication effects that may be causing conduction abnormalities. Postoperative atrial fibrillation occurs in 25-40% of open-heart surgery patients. The occurrence of atrial fibrillation places the patient at high risk for embolic cerebral infarcts, heart failure, cardiogenic shock, and ventricular arrhythmias. Patients undergoing open-heart surgery are often placed on amiodarone and beta-blockade following surgery to prevent atrial fibrillation.
Amiodarone is a Class III antiarrhythmic which prolongs the action potential, prolongs the refractory period, and affects the potassium channels. This has the effect of slowing the intracardiac conduction. It also has beta-blocker/calcium channel blocker like effects on the SA and AV node. A trial off of these medications should be done before placement of a PPM.
This patient was admitted for close cardiac monitoring. She continued to have symptoms after 2 days off amiodarone and beta-blockade, and therefore underwent an uncomplicated PPM implantation.
Key Readings
- Risk factors: Ann Thorac Surg 2008;85:108
- AFIST Trial: Lancet 2001;357:830.
Contribute your thoughts.